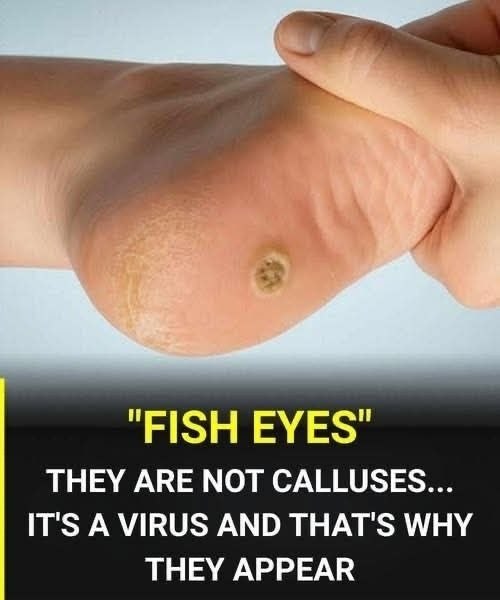
That rough patch on your sole might not be a callus. And treating it like one could make things worse. Let’s clarify the key differences—without fear-mongering—so you can care for your feet wisely.
The Core Difference: Friction vs. Virus
| Feature | Callus | Plantar Wart |
|---|---|---|
| Cause | Friction/pressure (shoes, standing) | HPV virus (types 1, 2, 4, 27, 57) entering through tiny skin breaks |
| Contagious? |  No No |  Yes—but requires direct contact + skin breach (not highly contagious) Yes—but requires direct contact + skin breach (not highly contagious) |
| Location | Pressure points (heel, ball of foot) | Anywhere on sole—often where virus entered |
| Texture | Uniformly thickened, yellowish | Rough, cauliflower-like; may have tiny black dots |
| Skin lines | Natural foot ridges continue through callus | Ridges disrupted or pushed aside by wart |
| Pain pattern | Hurts when pressed directly (standing) | Hurts when pinched from sides (lateral pressure) |
Key visual clue: Those “black dots” in warts aren’t seeds—they’re clotted capillaries (tiny blood vessels). Calluses have no dots.
Why Misidentifying Matters
Treating a wart like a callus can backfire:
-
- Filing/shaving removes surface skin but doesn’t kill the virus—may spread it to surrounding skin
- Moisturizing heavily creates a damp environment where HPV thrives
- Ignoring it lets the wart grow deeper (due to walking pressure) or spread to other areas
Good news: Most plantar warts resolve on their own within 1–2 years (65–70% clear spontaneously). Treatment speeds healing but isn’t always urgent—unless painful or spreading.
When to See a Doctor (Not Optional)
Seek professional care if you have:
-
Diabetes or poor circulation (foot injuries heal slower; risk of infection)
Weakened immune system (HIV, chemotherapy, immunosuppressants)
Wart bleeding, changing color, or growing rapidly
Pain interfering with walking
No improvement after 2–3 months of OTC treatment
Multiple warts spreading across foot
Never self-treat foot lesions if diabetic—even minor cuts can lead to serious complications.
Evidence-Based Treatment Options:
Evidence-Based Treatment Options
First-Line: OTC Salicylic Acid (Most Effective Home Treatment)
- How it works: Dissolves keratin (wart tissue) gradually
- Product: 17% salicylic acid pads/liquid (e.g., Compound W, Dr. Scholl’s)
- Method:
- Soak foot 5 mins in warm water
- Gently file wart surface with pumice after soaking (not dry!)
- Apply acid only to wart (protect surrounding skin with petroleum jelly)
- Repeat daily for 8–12 weeks
- Success rate: ~70% with consistent use
Second-Line: Cryotherapy (Freezing)
- At-home kits: Less effective than professional (weaker freezing temp)
- Doctor-performed: Liquid nitrogen application; may require 2–4 sessions
- What to expect: Blister forms, wart sloughs off in 1–2 weeks
Professional Options (For Stubborn Warts)
- Cantharidin (“beetle juice” paint-on blistering agent)
- Laser therapy
- Minor surgery (curettage)—rarely first choice (risk of scarring)
Avoid: Duct tape monotherapy (studies show no better than placebo), apple cider vinegar soaks (can cause chemical burns), or cutting warts yourself (infection risk).
 Prevention: Practical Steps That Actually Work
Prevention: Practical Steps That Actually Work
| Strategy | Why It Helps |
|---|---|
| Wear flip-flops in public showers/pools | HPV thrives on warm, damp surfaces—barrier prevents contact |
| Keep feet dry | Virus spreads more easily in moist environments; change socks if sweaty |
| Don’t pick/scratch warts | Spreads virus to other areas of your foot (“satellite warts”) |
| Cover existing warts with bandage | Reduces autoinoculation (spreading to yourself) |
| Don’t share towels/shoes | Lowers transmission risk to others (though casual contact rarely spreads HPV) |
Reality check: HPV is everywhere—most people encounter it. Warts develop only when virus enters and your immune system doesn’t clear it quickly. Not a hygiene failure.
FAQs: Your Questions, Answered
Q: Are plantar warts a sign of poor hygiene?
A: No. Anyone can get them—even with perfect foot care. Immune response matters more than cleanliness.
Q: Can I go swimming with a plantar wart?
A: Yes—but wear flip-flops in locker rooms/showers and cover the wart with a waterproof bandage while swimming.
Q: Why do warts hurt more when I pinch the sides?
A: Walking pressure pushes warts inward into sensitive tissue. Pinching from sides compresses nerve endings around the wart base.
Q: Will my wart come back after treatment?
A: Possible—the virus may linger. But immune system usually prevents recurrence. Reinfection from environment is rare.
Q: Are plantar warts related to genital HPV?
A: No. Different HPV strains cause plantar warts (types 1, 2, 4) vs. genital warts (types 6, 11) vs. cervical cancer (types 16, 18). No cross-transmission.
A Compassionate Perspective
Plantar warts are frustrating—but rarely dangerous. They’re not a reflection of your cleanliness or health habits. For most people, they’re a temporary nuisance that resolves with patience and consistent care.
If you’re diabetic or immunocompromised: see a podiatrist early—don’t wait.
If you’re otherwise healthy: Try OTC salicylic acid for 2–3 months. If no improvement, visit a doctor—not out of fear, but for peace of mind.
And remember: Your feet carry you through life. Treat them with kindness—whether the rough patch is a callus, a wart, or just life’s wear and tear.
“The best foot care isn’t about perfection. It’s about paying attention—with curiosity, not fear.”
Noticed a suspicious spot on your sole? When in doubt, show it to a podiatrist or dermatologist. A 5-minute exam beats months of guessing—and your feet will thank you.